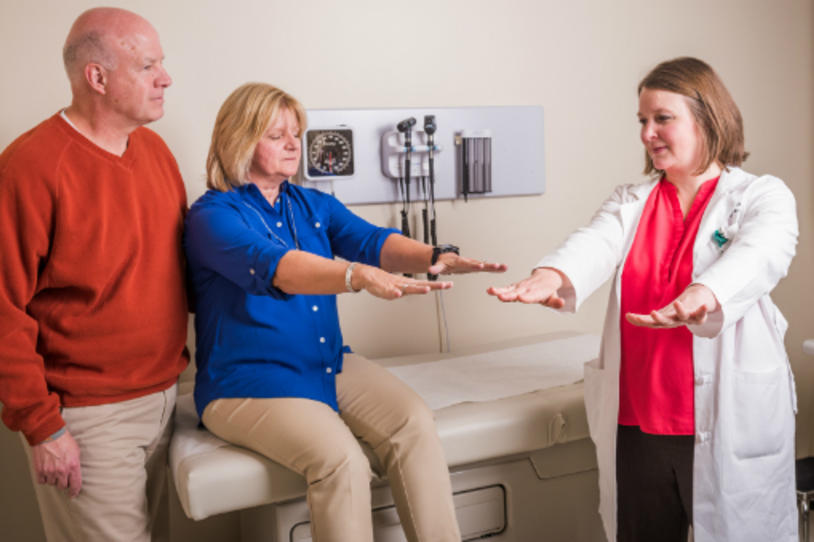
Physical therapists are a critical part of the Parkinson's care team. These experts can help you start or modify exercise to manage symptoms and potentially slow disease progression. And as Parkinson's progresses, they can work with you to adapt to new or changing symptoms. To learn more about physical therapy and its role in treating Parkinson's, I spoke with Gezel Villanueva-Fischberg, PT, MS, of Tamayo Physical Therapy in New York City.
Dr. Rachel Dolhun (RD): What is physical therapy?
Gezel Villanueva-Fischberg (GVF): Physical therapy (PT) is the treatment of a disease, injury or pain with specific exercises; physical agents such as heat, cold, light or ultrasound; mechanical devices; and other interventions rather than medications or surgery. PT isn't a substitute for medication or surgery, but it can help medication or surgery work better. (And medication or surgery can help PT work better, too.)
Physical therapy can treat any problem that impairs a person's ability to move and do their daily activities, such as walking, getting dressed or taking a shower. Physical therapists work with people of all ages, from newborns all the way to the elderly. My oldest patient was 102!
RD: What, exactly, does a physical therapist do?
GVF: At the first appointment, a physical therapist does a full examination, which includes many movement tests. We check how you get into and out of a chair, walk across the room, balance on one leg and move in many other ways. We look to see if there are walking changes, freezing, rigidity, dystonia or other symptoms. Sometimes I find things a patient doesn't notice. One woman came to me with handwriting problems but I found she had a shuffling gait.
Once we know where we're starting from, we develop a treatment plan. If there are gait problems, for example, we work on exercises to make steps bigger and improve coordination. If a person is falling, we'll figure out why (maybe they have an inactive lifestyle or weak core muscles) so that we can focus treatment on those areas. We always look at the whole person -- their symptoms, lifestyle, examination, goals -- to develop the best individual treatment.
RD: How can physical therapy help in Parkinson's?
GVF: Physical therapy can treat many symptoms at many stages of Parkinson's. In early and middle years, when people might have minimal symptoms, therapy can keep you ahead of symptoms you may not even recognize. I had one patient who told me, "I still garden and I don't know why my doctor sent me to you." When I did balance testing, we realized there were some problems, so we focused our attention there. In later stages, when there may be more trouble moving, a physical therapist can come to your home, do mobility exercises in a chair or bed, and teach you and your care partner how to change positions more easily.
Physical therapists use different methods and strategies for different symptoms. We use different types of cueing: visual, such as putting tape on the floor or having the patient look in a mirror; tactile, such as touching a body part to alert the patient to change direction; auditory, such as moving to the rhythm of music; and verbal, such as counting steps. I might have a patient take two steps to the right and two steps to the left with the beat of a metronome to improve coordination and balance. I also do a lot of dance to different music. This can help rigidity, because it makes a person separate their hips and lower body from their upper body. Boxing is another great exercise that improves coordination and range of motion. Different cues and exercises lessen symptoms and improve overall functioning and quality of life.
Whatever we do, we individualize the treatment to each patient's symptoms and current level of functioning. Some patients like dancing; others like boxing. No matter what we do, I challenge them. Sometimes, I combine strength and balance exercises to push people further. In some of my patients, I have them lift one leg while lifting a weighted ball with their arms, for example, instead of doing each exercise individually.
RD: When should you see a physical therapist?
GVF: As soon as possible after your diagnosis! Even if you aren't sure about your diagnosis -- say you are getting a second opinion or wondering if you have Parkinson's or another movement disorder -- try physical therapy. You can do PT at any time during life with Parkinson's, even when medications and other treatments seem to be working well. It's never too early or too late. It can't harm you. It can only improve your movement and your quality of life.
RD: How does physical therapy differ from occupational therapy?
GVF: It's very common for people to see physical, occupational and even speech therapists at the same time. I am a big proponent of all three. We work as a team to treat Parkinson's movement problems in slightly different ways. Physical and occupational therapists do a lot of the same things. PT may focus more on bigger movements, such as walking and balance, whereas occupational therapy looks at smaller movements such as buttoning your shirt or holding a knife to cut your food. Occupational therapists also can help with adaptive equipment, such as utensils for easier eating or a lift to get up from a chair more easily. And if necessary occupational therapists can do cognitive (memory and thinking) exercises.
Physical and occupational therapists both look at how symptoms affect daily life to develop and deliver personalized treatments.
RD: How do you find a physical therapist?
GVF: Ask your doctor or other people with Parkinson's for a recommendation. Or look online for one in your area. The American Physical Therapy Association maintains a database of physical therapists as does LSVT (Lee Silverman Voice Treatment) Global, a Parkinson's specific program.
While you'll need a doctor's prescription for ongoing PT, you may not need one to get started. In New York State, for example, patients can see a physical therapist without a referral for 30 days or 10 visits, whichever comes first. Rules and regulations vary by state and insurer.
Although most insurance companies cover physical therapy, it may be good to ask your insurer whether there are out-of-pocket costs and in-network providers. Sometimes these aren't Parkinson's experts, but they can still help.
Be sure to ask your therapist about their credentials, background, and experience with Parkinson's and other movement or neurological disorders. And if you aren't happy with your first physical therapist, find another.
RD: What else should people know about physical therapy?
GVF: Physical therapy is a good way for people to be active and take control in their disease. Especially early on, many people feel they are losing control and sometimes give up on activities that give them pleasure. I had one patient who thought he had to stop golfing because of his Parkinson's but I told him, "We can work on that!" We can work on rotation for golf, coordination for dancing or boxing, or whatever you enjoy doing. It's so important to keep doing the things you love, and physical therapy can help you.
Physical therapists are coaches. We aren't just prescribers who tell you that you "have to do this or that." We want you to get involved in your treatment, to take ownership and responsibility so that you want to do it, and it's a partnership. We want you to think, for example, "I want to take a nap, but my therapist told me to do my exercises and I know how important they are for my balance."
We're big on education, on helping people understand and accept what they are going through so we can help them move through it. Together, we can improve your life.
